Essential Guide to Routine Testing for Legionella in 2026
1. Introduction:
Legionella outbreaks are on the rise, posing serious risk to public health across hospitals, hotels, office buildings, and other water systems. According to the CDC, the number of reported Legionnaires' disease cases in the U.S. has nearly tripled since the early 2000s, and global trends suggest a similar upward trajectory. These bacteria thrive in complex water systems, where even a small lapse in monitoring can lead to rapid contamination and spread of disease.
The consequences of an outbreak extend far beyond health impacts. A single case can trigger lengthy investigations, facility closures, costly remediation, and damage to an organization's reputation. In 2015, more than 5000 cases of legionellosis were reported to the Centers for Disease Control and Prevention (CDC) which is a 4-fold increase from 2001.
This escalating risk highlights the critical need for proactive, routine Legionella testing. Waiting until an outbreak occurs can have severe health and operational consequences. Facilities must act preemptively by identifying potential hazards and addressing them before they pose a threat to residents, employees, or visitors. By incorporating structured testing protocols into a comprehensive Water Management Plan (WMP), organizations can detect Legionella early, track system performance over time, and ensure their water systems remain both safe and compliant with public health guidelines.
In this guide, we explore the essentials of Legionella, the critical role of routine testing, and practical strategies for implementing effective testing programs in 2026 and beyond.
2. Understanding Legionella:
2.1. What is Legionella?
Legionella is a genus of Gram-negative, aerobic bacteria commonly found in natural and man-made aquatic environments. They are frequently detected in complex water systems such as potable water plumbing networks, hot water tanks, cooling towers, spas, and fountains where water may stagnate or form aerosols. These bacteria can colonize biofilms lining pipes, valves, and other surfaces, allowing them to persist and multiply even under routine disinfection conditions.
Certain species, particularly Legionella pneumophila, are opportunistic pathogens that cause Legionnaires' disease, a severe and potentially life-threatening form of pneumonia characterized by fever, cough, and respiratory distress. Other species can cause Pontiac fever, a self-limiting, flu-like respiratory illness without pneumonia. Humans become infected primarily through inhalation of aerosolized water droplets containing viable bacteria. This makes proactive water system monitoring and control essential to prevent outbreaks in healthcare facilities, commercial buildings, and residential settings.
2.2. How it spreads:
- Inhalation of aerosolized water droplets: Legionella bacteria are primarily transmitted to humans through inhalation of aerosolized water droplets that contain viable organisms. These tiny droplets can be generated by a variety of water systems, including faucets, showers, cooling towers, humidifiers, and decorative fountains. When inhaled, the bacteria can reach the lower respiratory tract and infect the lungs, potentially leading to Legionnaires' disease.
- Exposure in warm water environments: Individuals can become exposed through direct contact with contaminated water sources such as hot tubs, spas, and showerheads. These environments provide warm temperatures and stagnant water conditions that promote bacterial growth, creating a higher risk of infection for users.
- Aspiration of contaminated water: Although less common, aspiration of contaminated water can also introduce Legionella into the lungs, resulting in respiratory illness. This may occur during medical procedures, in elderly or debilitated individuals, or through accidental inhalation.
Understanding these pathways is critical for designing effective water management and routine testing strategies to reduce exposure risk in healthcare, commercial, and residential settings.
2.3. Public Health and Operational Impact:
Legionella infections pose serious health risks, particularly for vulnerable populations such as the elderly, individuals with weakened immune systems, patients with chronic lung conditions, and those with underlying medical comorbidities. These groups are more susceptible to severe respiratory illness, prolonged hospitalization, and complications that can be life-threatening.
Beyond individual health concerns, Legionella outbreaks have significant operational and economic consequences. Facilities experiencing an outbreak may face temporary closures, emergency remediation measures, regulatory investigations, and reputational damage.
2.4. Real-world impact:
Legionella outbreaks continue to illustrate the serious health and operational consequences when water systems are not effectively managed. Recent events show that even large urban centers and healthcare facilities remain vulnerable without robust monitoring and control measures.
- Central Harlem, New York City: A Legionnaires' disease outbreak between July and August 2025 resulted in more than 110 confirmed cases and at least six deaths, with multiple hospitalizations linked to Legionella contamination across several buildings, including a city-run hospital and clinic.
- England and Wales: Surveillance data reported 472 cases of legionellosis in 2024, with nearly two-thirds of infections occurring in adults aged 60 years and older, underscoring persistent risk among older populations and the ongoing need for vigilance in water management.
- Elsewhere in the U.S., clusters of Legionnaires' disease have been investigated in locations such as Marshalltown, Iowa, where reported cases included vulnerable individuals and prompted public health alerts.
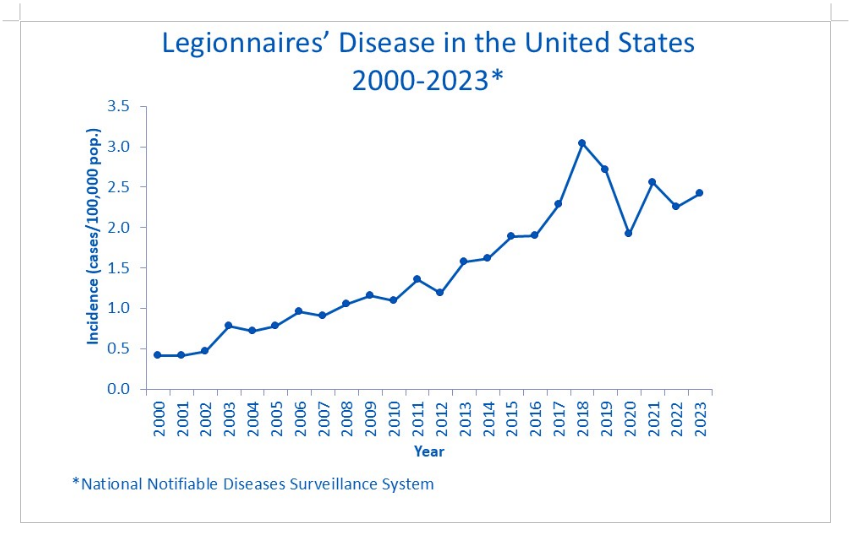
Figure 1. Incidence of Legionnaires' Disease in the United States, 2000–2023
Observed Trend: Between 2000 and 2010, the incidence of Legionnaires' disease remained relatively low, generally below 1.5 cases per 100,000 population. From 2010 onwards, there is a clear upward trend, with a peak in 2018 reaching approximately 3.0 cases per 100,000 population. After 2018, incidence fluctuates slightly but continues to remain elevated compared to the early 2000s, indicating a sustained increase over the last two decades.
Significance: The rising incidence reflects a growing public health concern related to Legionella bacteria. This trend underscores the importance of proactive water management, routine testing, and preventive measures in high-risk settings such as hospitals, hotels, and cooling towers. The data highlights the need for facilities to implement structured Legionella monitoring protocols and validated Water Management Plans (WMPs) to reduce outbreak risks and protect public health.
Data Source: National Notifiable Diseases Surveillance System (NNDSS), United States Centers for Disease Control and Prevention (CDC) (https://www.cdc.gov/legionella/php/surveillance/index.html)
3. The Importance of Routine Testing:
3.1. Significance of Routine Legionella Testing:
By incorporating routine testing into daily operations, facilities can move from a reactive approach to a proactive strategy, identifying potential risks before they escalate into outbreaks. This not only helps protect the health of residents, patients, and staff but also provides actionable insights that inform maintenance, disinfection, and water management practices. Consistent monitoring establishes a clear understanding of system performance over time, enabling organizations to make data-driven decisions and validate the effectiveness of their Water Management Plans.
3.1.1. Establishing Performance Benchmarks:
Routine monitoring enables facilities to establish baseline Legionella concentrations across key water system components, including cooling towers, hot water tanks, and plumbing networks. Continuous tracking of these levels allows organizations to:
- Identify trends or unexpected changes in bacterial loads.
- Detect early colonization before it develops into a full-scale outbreak.
- Assess the efficacy of existing control measures, including temperature regulation, disinfectant dosing, and system flushing.
By providing these quantitative benchmarks, routine testing supports evidence-based evaluation of system performance and facilitates informed decision-making for maintenance, remediation, and ongoing risk management.
3.1.2. Validation of Water Management Plans (WMPs):
A Water Management Plan outlines preventive measures, monitoring protocols, and corrective actions for controlling Legionella growth. Routine testing is essential for validating these plans because it:
- Confirms that preventive controls, such as disinfection schedules and temperature maintenance, are working effectively.
- Provides data-driven evidence for compliance with public health regulations and industry standards.
- Helps refine WMP procedures based on observed microbial trends and risk assessments.
For example, a healthcare facility implementing monthly Legionella testing in high-risk outlets was able to validate its WMP controls, detecting minor bacterial increases early and performing targeted remediation before an outbreak occurred.
By integrating routine testing into a WMP, organizations can reduce the likelihood of Legionella proliferation, protect high-risk populations, and maintain regulatory compliance, making routine testing both a preventive and quality assurance measure.
4. Implementation Strategies:
Effective control of Legionella spp. requires a structured, proactive approach encompassing routine monitoring, validated testing methodologies, and trained personnel. HiMedia Labs provides advanced solutions to support the implementation of standardized testing protocols and ensure water system safety.
4.1. Structuring Routine Testing Protocols:
Facilities should establish a risk-based routine testing schedule. High-risk water systems, including cooling towers, hot water storage tanks, and healthcare outlets, require monthly or quarterly testing. Low-risk systems may follow a semi-annual schedule.
Critical sampling points should be identified through a comprehensive system assessment, focusing on locations with a higher likelihood of bacterial colonization, such as faucets, showerheads, storage tanks, and recirculation loops. Each sampling point should be documented within the Water Management Plan (WMP) to maintain consistency in monitoring.
Sample collection should follow standardized procedures using HiMedia sterile sampling bottles. Metadata including location, collection time, and water temperature must be recorded to ensure data reliability and reproducibility.
4.2. Application of Modern Testing Methodologies
HiMedia offers a suite of products for reliable detection and quantification of Legionella spp.
- Culture-Based Methods: HiMedia Legionella Selective Agar supports selective growth and enumeration of Legionella species, providing quantitative data essential for performance benchmarking.
- Molecular Detection Methods: PathoSEEK® Legionella Molecular Kits enable rapid and highly sensitive detection of Legionella DNA, facilitating early intervention prior to significant bacterial proliferation.
- Combined Approaches: Integrating culture-based and molecular assays delivers both accuracy and rapid turnaround, supporting timely corrective actions and long-term monitoring of water systems.
4.3. Personnel Training and Competency:
Personnel must be trained in standardized sampling, testing methodologies, and documentation practices. HiMedia provides detailed protocols and training resources for both culture-based and molecular testing.
Clearly defined responsibilities for monitoring, testing, and corrective interventions ensure accountability and reduce operational gaps.
Maintaining standard operating procedures and training logs reinforces best practices and ensures procedural consistency among staff.
5. Practical Checklist: Essential Steps for Effective Legionella Testing
Implementing a robust Legionella monitoring program requires both planning and consistency. The following checklist provides actionable steps and key considerations to ensure effective testing and risk mitigation:
5.1. Evaluate Your Water Management Plan (WMP):
Ask critical questions to assess your WMP:
- Does the plan clearly identify all high-risk water systems and outlets?
- Are routine testing frequencies aligned with the risk level of each system?
- Are corrective actions predefined for elevated Legionella levels?
- Is staff training documented and regularly updated?
- Are sampling and testing protocols standardized and validated?
- Are records of past testing results maintained for trend analysis?
- Are regulatory compliance requirements incorporated into the WMP?
- Are modern detection methods, such as PathoSEEK® molecular kits, utilized alongside culture-based approaches?
5.2. Define Sampling Strategy:
- Identify critical sampling points, including cooling towers, storage tanks, faucets, and showers.
- Use HiMedia sterile sampling bottles to ensure sample integrity.
5.3. Implement Validated Testing Methods:
- Utilize HiMedia Legionella Selective Agar for culture-based enumeration.
- Employ rapid molecular detection using PathoSEEK® Legionella Molecular Kits for early identification.
- Consider a combined testing approach to balance accuracy and speed.
5.4. Maintain Data Records and Trend Analysis:
- Record all test results systematically.
- Use results to establish baseline Legionella concentrations.
- Track trends to detect early signs of colonization and evaluate the effectiveness of preventive measures.
5.5. Conduct Staff Training and Assign Responsibilities:
- Train personnel in sample collection, testing, and documentation protocols.
- Clearly define roles for monitoring, corrective actions, and data review.
- Maintain SOPs and training logs to ensure procedural consistency.
5.6. Review and Update Protocols Regularly
- Periodically assess and refine the WMP based on monitoring data.
- Integrate emerging technologies and best practices for Legionella control.
5.7. Communicate Findings and Promote Awareness
- Share testing results with relevant stakeholders.
- Use findings to support facility audits, compliance reporting, and continuous improvement initiatives.
6. Conclusion:
Routine Legionella testing is a critical component of effective water management. By implementing structured sampling protocols, utilizing validated testing methods, and ensuring staff competency, facilities can detect early colonization, prevent outbreaks, and maintain regulatory compliance. Integrating advanced HiMedia products, such as Legionella Selective Agar and PathoSEEK® molecular kits, enables accurate and rapid detection, supporting evidence-based decision-making.
A proactive, data-driven approach to monitoring not only protects residents, patients, and staff but also strengthens facility confidence in their water management program. Establishing baseline microbial levels, tracking trends over time, and validating your Water Management Plan ensures continuous improvement and sustains public health safety.
7. Call to Action:
- Protect your facility from Legionella risks today. Explore HiMedia Labs comprehensive solutions for routine Legionella testing and water system monitoring: www.himedialabs.com/us
- Request personalized guidance from our experts to tailor a testing program for your facility: infous@himedialabs.com
- Subscribe to our newsletter for ongoing insights, case studies, and best practices in water safety and Legionella control.
- Learn more about our products, including culture media and molecular kits, to enhance your water management strategy.
- Stay informed. Stay prepared. Ensure water safety with HiMedia Laboratories Pvt Ltd.